Det har været mærkeligt lige fra starten. Hvis SARS-CoV-2 (den nye coronavirus, der forårsager Covid-19) bruger det angiotensin-konverterende enzym 2 (ACE2) som en receptor til at inficere celler, hvorfor er det så en lungesygdom, når lungerne har lave niveauer af ACE2? Dette blev bestemt tilbage i maj 2020 i en undersøgelse, der fandt, at alveolær celle type 2 (det primære mål for SARS-CoV-2) i lungerne har ACE2-ekspression, der er '4,7 gange lavere end det gennemsnitlige ekspressionsniveau for alle ACE2-udtrykkende celletyper ,' såsom lever, mave, ileum, nyre og tyktarm.
Kommentar: Delvist oversat af Sott.net fra ACE2 isn't solely responsible for Covid-19, which explains a lot
Later, a systematic review published over a month ago further points out that SARS-CoV-2 tend to end up in places not consistent with ACE2 expression levels. Looking at the figure below, organs SARS-CoV-2 tend to localize (e.g., lungs and brain) do not always have high expression of ACE2, and vice-versa.
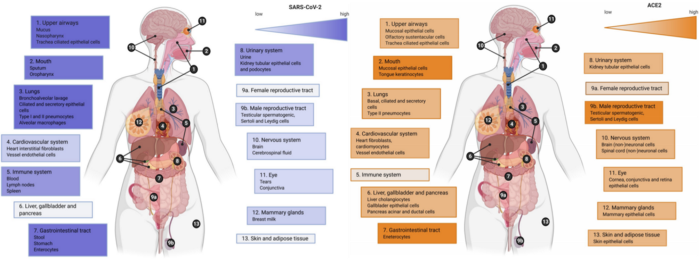
Right: Gradient color (orange) indicates low to high evidence for ACE2 expression; the highest expression was detected in the oral cavity, gastrointestinal tract, and the male reproductive system.
Neuropilin-1
In 2009, a study discovered that neuropilin-1 could bind to genes with patterns conforming to the C-end rule. Apparently, the genetic sequence of SARS-CoV-2 spike protein also has this C-end rule.
So, two independent groups of international researchers sought to test if SARS-CoV-2 could use neuropilin-1 as a receptor. The resulting two papers were published last month in Science with the titles, "Neuropilin-1 facilitates SARS-CoV-2 cell entry and infectivity," and "Neuropilin-1 is a host factor for SARS-CoV-2 infection." Judging from the titles alone, we know the hypothesis is confirmed to be true.
In short, they showed that SARS-CoV-2 can still infect cells deficient in ACE2, as long as they express neuropilin-1. If both ACE2 and neuropilin-1 receptors are present, the infection became more infectious. Using genetic editing to cut or antibodies to block neuropilin-1, in turn, prevent SARS-CoV-2 infection.
"Whereas ACE2 was detected at very low levels, [neuropilin-1] were abundantly expressed in almost all pulmonary and olfactory cells, with the highest levels of expression in endothelial cells."Binding to neuropilin-1 would hinder its normal function, which is to aid neurons to make connections and blood vessels to grow. This explains why SARS-CoV-2 can attack the nervous and vascular systems. This explains why Covid-19 is also a neurological and vascular disease. And why SARS-CoV-2/Covid-19 attacks the lungs and sense of smell since neuropilin-1 is highly expressed in the respiratory and olfactory tracks.
As one of the studies in Science stated:
"Whereas ACE2 was detected at very low levels, [neuropilin-1] were abundantly expressed in almost all pulmonary and olfactory cells, with the highest levels of expression in endothelial cells."Endothelial means blood vessels; thus, neuropilin-1 concentrates in blood vessels and cells of the lungs and nose. This study also did an autopsy of olfactory cells isolated from the nose of deceased Covid-19 victims, showing that cells positive for neuropilin-1 — but lacking ACE2 — were still infested with SARS-CoV-2 particles.
Interestingly, another research group had found that rats with chronic neuropathic pain no longer feel pain when the spike protein of SARS-CoV-2 blocked neuropilin-1. This is because neuropilin-1 participates in pain excitation in neurons. In an anecdote, a 49-year-old South African male suffered a nerve injury in a motor accident in 2011. As a result, he lived with chronic pain — so unbearable that it disrupts his sleep every night — until he got Covid-19.
"I found it very strange: When I was sick with Covid, the pain was bearable. At some points, it felt like the pain was gone. I just couldn't believe it," he said. "I lived a better life when I was sick because the pain was gone." But the man recovered from Covid-19, and his pain resurfaced.CD147 (Basigin)
This month, a new study was published in the Nature-partnered journal, Signal Transduction and Targeted Therapy, titled "CD147-spike protein is a novel route for SARS-CoV-2 infection to host cells." Again, the title has said it all. Researchers in China discovered that SARS-CoV-2 could infect human cells and mice expressing CD147 (also called basigin). SARS-CoV-2 infection can be further blocked with Meplazumab (an anti-CD147 antibody) or boosted with increasing CD147 expression.
"These findings demonstrate that CD147 provides more entries for SARS-CoV-2 infection and plays a potential role in mediating virus infection, especially in ACE2-deficient cell types."More importantly, this study showed that T-cells (both CD4+ and CD8+) collected from human blood were susceptible to SARS-CoV-2 infection via CD147. Notably, the study also confirmed that these T-cells do not express the ACE2 receptor, which is expected as T-cells are inherently ACE2 deficient.
The T-cell's CD147 functions as a receptor to receive chemotaxis signals. Chemotaxis is the attraction or recruitment of immune cells to the area where foreign invaders are located. Thusly, CD147 expression heightens when T-cells are activated. As follows, in the above study, activated T-cells were also shown to be more susceptible to SARS-CoV-2 infection than inactive T-cells. This also explains why Covid-19 tends to reduce T-cell count in severe cases.
In addition, the study determines the levels of ACE2 and CD147 expressions in human lung cells — BEAS-2B, and Vero E6 bronchial cells. Apparently, CD147 expression was 2.3-fold higher than ACE2 in Vero E6 cells, and ACE2 wasn't even expressed in BEAS-2B cells.
"These findings demonstrate that CD147 provides more entries for SARS-CoV-2 infection and plays a potential role in mediating virus infection, especially in ACE2-deficient cell types," the study authors wrote.Exploiting the CD147 receptor is not unique to SARS-CoV-2. It's also a receptor that the human immunodeficient virus type 1 (HIV-1) — that causes AIDS — uses. As T-cells are important for the specialized killing of infection, it's not unexpected that viruses evolve ways to counter T-cells.
Short abstract
We thought ACE2 is the only receptor SARS-CoV-2 can use for almost a year, which is odd given that the lungs don't even have a high ACE2 expression. But in the past month, two additional receptors of SARS-CoV-2 were discovered. One is neuropilin-1, which is highly expressed in the respiratory and olfactory tracts, specifically in cell types that SARS-CoV-2 preferentially infects. The second is CD147 (also called basigin), which is highly expressed in T-cells and bronchial cells in the lungs. This clarifies why Covid-19 tends to kill certain lung cells and T-cells that don't have ACE2.
Overall, these two newly identified receptors of SARS-CoV-2 explain many facets of Covid-19 that ACE2 alone cannot. We now know why Covid-19 is a mix of pulmonary, vascular, neurological, immunological, and olfactory diseases.



Kommentar: See also: